.webp)
Revenue cycle management: The AI strategy pitfall
Most AI strategies in revenue cycle will fail. Here’s why.
Health systems are investing aggressively in automation and revenue cycle management to protect margins. Most will see limited return. The issue is not the technology. It is the operating model behind it and how healthcare revenue cycle leaders use healthcare data analytics to drive change.
.webp)
The revenue problem is not cyclical; it’s structural
Health systems are operating inside a financial vice.
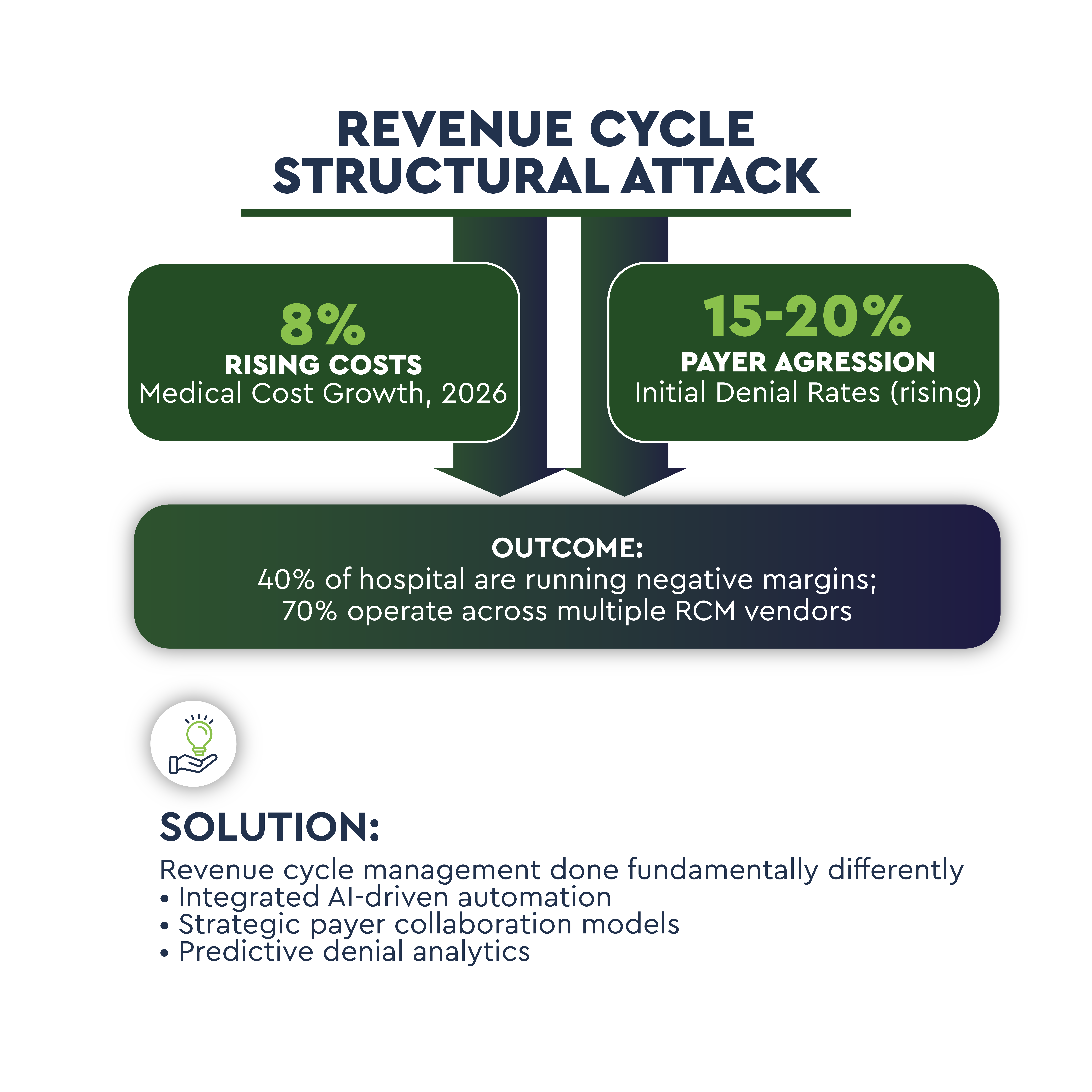
Costs are rising. Medical cost growth is projected to reach 8% in 2026. At the same time, revenue per discharge is under pressure, and nearly 40% of hospitals are running negative margins. As acuity shifts and emergency department volumes fluctuate, volume growth can no longer mask inefficiency. That lever is gone.
Payers have changed the rules. They are deploying AI to scale denials and automate medical necessity reviews. Initial denial rates now range from 15% to 20%, and they are rising.
The result is a structural shift. Revenue cycle management (RCM) is no longer a back-office function. It is one of the few remaining levers for financial survival, and it must be supported by robust revenue cycle analytics and healthcare data analytics.
For revenue cycle leaders, the goal has shifted from incremental collections to preserving net patient service revenue (NPSR) and protecting solvency across the healthcare revenue cycle.
Most organizations understand this. Where they go wrong is how they respond.
Technology alone will not fix a broken operating model
The prevailing approach is straightforward: invest in automation, layer in AI, and expect efficiency to follow.
It usually doesn’t.
The issue isn’t what the technology can do. It’s how it gets deployed. Most health systems try to solve a structural problem with point solutions by automating pieces of a fragmented RCM system and expecting enterprise impact.
And with structural labor shortages, performance can no longer be a function of adding headcount. Capacity is capped.
The data reflects the outcome. Nearly 70% of hospitals operate across multiple RCM vendors. Workflows remain disconnected, the patient experience is inconsistent, and administrative waste persists. Automation applied to fragmentation does not create efficiency. It scales dysfunction.

This is where most AI strategies fail. They optimize tasks, not systems, and they rarely leverage revenue cycle analytics or broader healthcare data analytics to redesign the healthcare revenue cycle end-to-end.
The advantage will come from hybrid operating models
Organizations that are outperforming are doing something most won’t: they are not starting with tools; they are redesigning how work gets done across the cycle.

This is the shift to a hybrid operating model.
In this model, AI is not the strategy; it’s the execution engine. It handles high-volume, rules-based work with speed and consistency. However, it remains tightly integrated with operational expertise that redesigns workflows, manages exceptions, and drives accountability using revenue cycle analytics and healthcare data analytics.
That combination changes the outcome.
Instead of reacting to denials, organizations begin to predict and prevent them. Instead of scaling labor to manage volume, they redesign processes to reduce it. Instead of layering vendors, they integrate workflows across EMRs, payers, and key partners to strengthen the healthcare revenue cycle.
The impact is immediate and measurable. High-friction work, such as prior authorization, eligibility, and denials, starts to produce near-term gains in NPSR while the organization builds the foundation for longer-term transformation of RCM.
This is not a technology upgrade. It is an operating model shift for the entire healthcare revenue cycle.
One way to operationalize the hybrid model is a bridge strategy. It is a hybrid operational-IT approach that delivers near-term relief while preparing for longer-term platform maturity.
- Drive immediate ROI by going after the work that is bleeding time, cash, and capacity (front-end integrity, clinical documentation capture, and workforce constraints).
- Build integration-ready architecture that plays cleanly with the EHR, so you are not re-platforming the same workflows again when native capability catches up.
- Deploy adaptive intelligence that learns payer behavior, flags drift early, and adjusts as policies and regulations shift.
The decision facing healthcare leaders is clear
Health systems can continue to absorb payer inefficiency through labor and incremental automation, or they can redesign revenue operations around a model that combines AI, revenue cycle analytics, and disciplined execution across revenue cycles.
The difference is not subtle. One approach preserves the status quo under increasing pressure. The other builds a durable advantage in the healthcare revenue cycle.
The organizations that move now will not just stabilize margins. They will change how revenue is generated, protected, and scaled.
The question is not whether to invest in AI. It is whether you are willing to change the system it operates within, and whether you will use healthcare data analytics and revenue cycle analytics to make that change stick.

Meet the Author